MR-proADM in the ED: Early identification of disease progression to sepsis
Study finds that the blood biomarker MR-proADM most accurately identifies the patients with suspected infection and a high likelihood of further disease progression
The recently published study (The early identification of disease progression in patients with suspected infection presenting to the emergency department with MR-proADM, Saeed et al. Critical Care (2019) 23:40) concluded that in patients presenting to the emergency department (ED) with suspected infection, the biomarker MR-proADM could most accurately identify the likelihood of disease progression. Incorporation of MR-proADM into an early sepsis management protocol may therefore aid rapid decision-making in order to either initiate, escalate or intensify early treatment strategies, or identify patients suitable for safe out-patient treatment.
Video: Integration of B·R·A·H·M·S MR-proADM KRYPTOR into clinical risk assessment in the ED
Dr Kordo Saeed presents his observational study comparing different risk assessment tools in the Emergency Department.
This study proposes two clinically important uses for MR-proADM in the emergency department (ED):
- An early escalation of treatment in patients with MR-proADM concentrations ≥ 1.5 nmol/L, thus identifying an already high level of disease severity or a high potential for further development and progression
- A decreased number of hospital admissions allowing a safe increase in out-patient treatment in patients with MR-proADM concentrations < 0.9 nmol/L
MR-proADM is most useful in patients with few pathophysiological signs and symptoms
MR-proADM measurement at presentation in the emergency department could accurately assess disease severity and identify specific patient populations based on the likelihood of subsequent disease progression to sepsis. This is of particular importance in patients with few pathophysiological signs and symptoms, as indicated by low SOFA, qSOFA or NEWS scores, where initial treatment may either be withheld, delayed or insufficient.
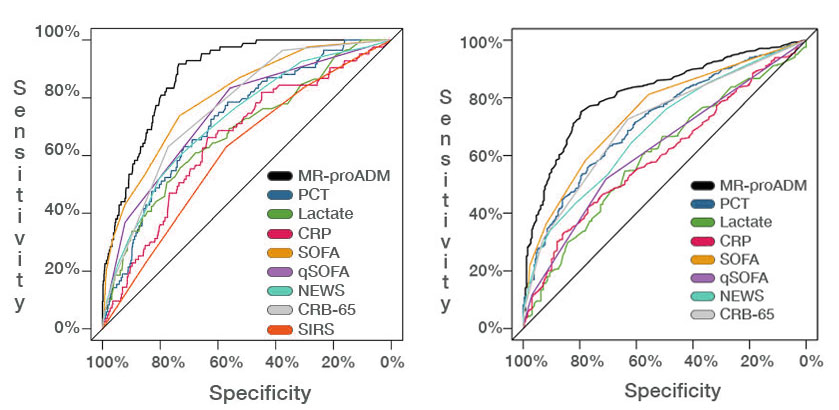 Receiver Operating Characteristics (ROC) curves for 28-day mortality prediction (left) and for hospitalization decisions (right) in patients presenting with clinical suspicion of infection to the emergency department (ED).
Receiver Operating Characteristics (ROC) curves for 28-day mortality prediction (left) and for hospitalization decisions (right) in patients presenting with clinical suspicion of infection to the emergency department (ED).
(CRB-65 severity score for community-acquired pneumonia, CRP C-reactive protein, MR-proADM mid-regional proadrenomedullin, NEWS National Early Warning Score, PCT procalcitonin, qSOFA quick Sequential Organ Failure Assessment, SIRS systemic inflammatory response syndrome, SOFA Sequential Organ Failure Assessment)
Adapted from Saeed et al. Critical Care (2019) 23:40
MR-proADM helps to triage patients to initiate appropriate treatment in the ED
Patients with MR-proADM concentrations above ≥ 1.54 nmol/L but low values for other biomarkers or low clinical scores had longer length of hospitalization, higher rate of ICU admission, elevated mortality risk and a greater number of disease progression events.
Conversely, the presence of low biomarker values, clinical scores and MR-proADM concentrations < 1.54 nmol/L resulted in identification of a high number of uncomplicated infections with low mortality rates, low ICU admission rates, low lengths of hospitalization.
This study highlights the use of MR-proADM in potentially identifying this patient population in order to initiate appropriate treatment strategies at the earliest opportunity.
MR-proADM values < 0.87 nmol/L identify patients who could be treated in out-patient settings
Using MR-proADM values < 0.87 nmol/L could decrease the number of hospital admissions. In this low severity group no mortality and no increase in readmissions occurred. Such MR-proADM guidance in the ED could reduce unnecessary hospitalization of patients with uncomplicated infections who are at no further risk of disease progression, thus, leading to decrease in clinical workload and financial burden.
Conventional “real-life” hospital triage decisions compared with virtual MR-proADM guided triage decisions
1175 patients were analysed with respective 28-day mortality rates of 7.1%, and hospitalization rates of 77.9%. MR-proADM showed greatest accuracy in predicting 28-day mortality and hospitalization requirement.
- Increased out-patient treatment (15%) could be facilitated using a MR-proADM cut-off < 0.87 nmol/L, with decreased readmission rates and no mortalities
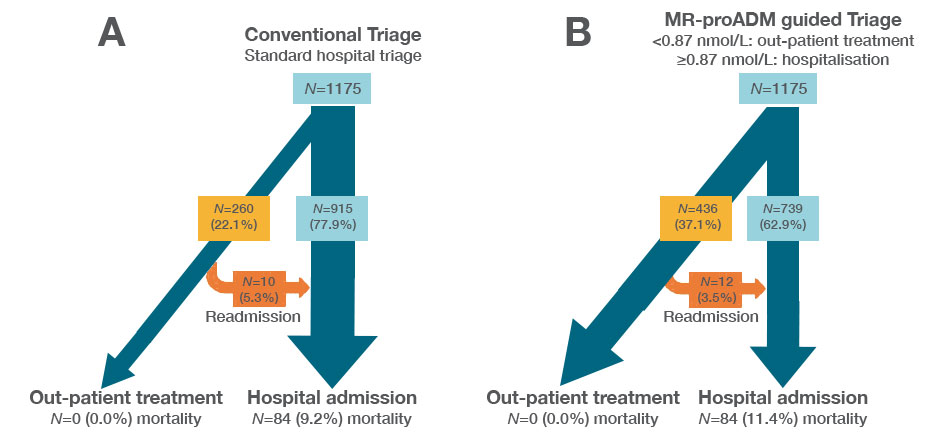 Patient triage decisions illustrating hospitalisation and out-patient treatment decisions after initial emergency department assessment, with corresponding mortality and re-hospitalization rates. (Panel A): conventional “real-life” hospital triage decisions, and (Panel B): virtual MR-proADM guided triage decisions.
Patient triage decisions illustrating hospitalisation and out-patient treatment decisions after initial emergency department assessment, with corresponding mortality and re-hospitalization rates. (Panel A): conventional “real-life” hospital triage decisions, and (Panel B): virtual MR-proADM guided triage decisions.
Adapted from Saeed et al. Critical Care (2019) 23:40
- Patient subgroups with high MR-proADM concentrations (≥ 1.54 nmol/L) and low biomarker (PCT < 0.25 ng/mL, lactate < 2.0 mmol/L or CRP < 67 mg/L) or clinical score (SOFA < 2 points, qSOFA < 2 points, NEWS < 4 points or CRB-65 < 2 points) values were characterized by a significantly longer length of hospitalization (p < 0.001), rate of ICU admission (p < 0.001), elevated mortality risk (e.g. SOFA, qSOFA and NEWS HR [95%CI], 45.5 [10.0–207.6], 23.4 [11.1–49.3] and 32.6 [9.4–113.6], respectively) and a greater number of disease progression events (p < 0.001), compared to similar subgroups with low MR-proADM concentrations (< 1.54 nmol/L)
